Other Opportunities
Fibrosis
Inflammation
Atherosclerosis
Oncology
Bone Defects
Infections
Fibrosis
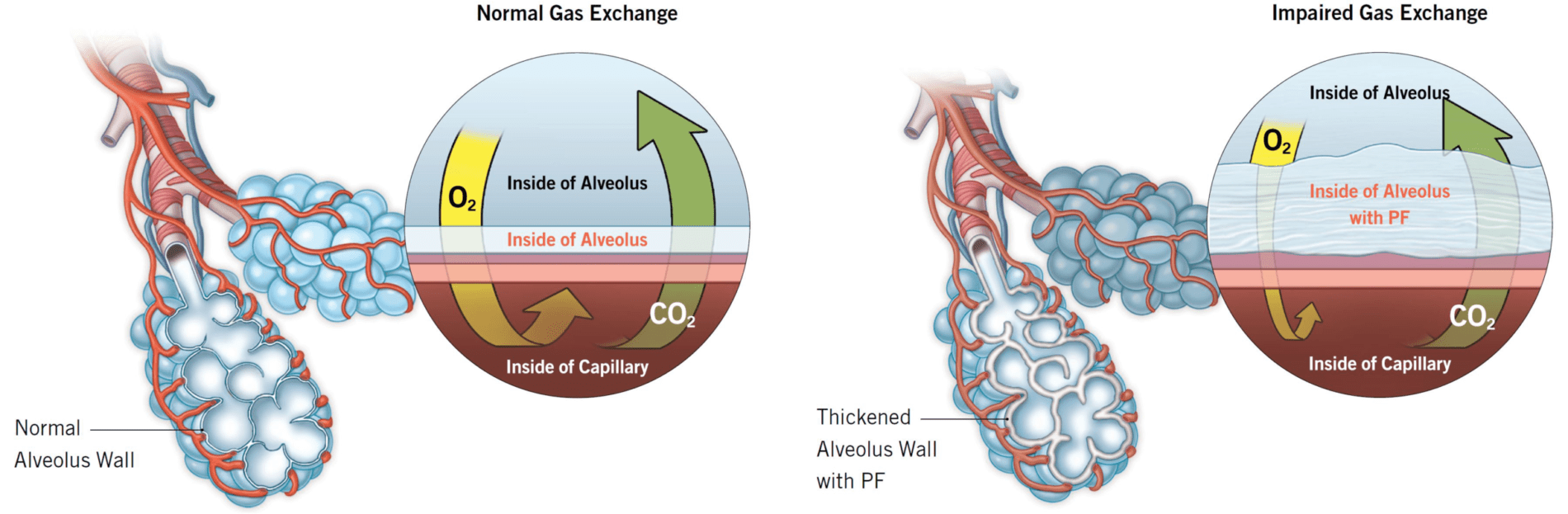
Idiopathic Pulmonary Fibrosis (IPF) is a chronic interstitial lung disease characterized by progressive, irreversible scarring of lung tissue and declining lung function, terminating in respiratory failure and ultimately death. The incidence of IPF is age related; the majority of IPF patients are over 60 years of age and this disease carries a high burden of morbidity and mortality with median patient survival limited to 3-5 years post diagnosis. There are currently two FDA-approved therapies, pirfenidone and nintedanib, both of which only slow the progression of the disease, mainly by curbing the decline of forced vital capacity (FVC) in IPF patients. However, since their introduction to the clinic in 2014, pirfenidone and nintedanib drug treatment, used alone or in combination, has not greatly reduced IPF mortality or significantly improved quality of life in IPF patients, highlighting the need for better understanding of IPF disease processes and the identification of new IPF drug candidates. Currently the only cure for IPF is lung transplantation.
According to the National Institutes of Health, IPF has an estimated prevalence of 13 to 20 per 100,000 people worldwide. An estimated 100,000 people are affected in the United States with 30,000 to 40,000 new cases being diagnosed each year, and as many as 40,000 Americans die from IPF each year.
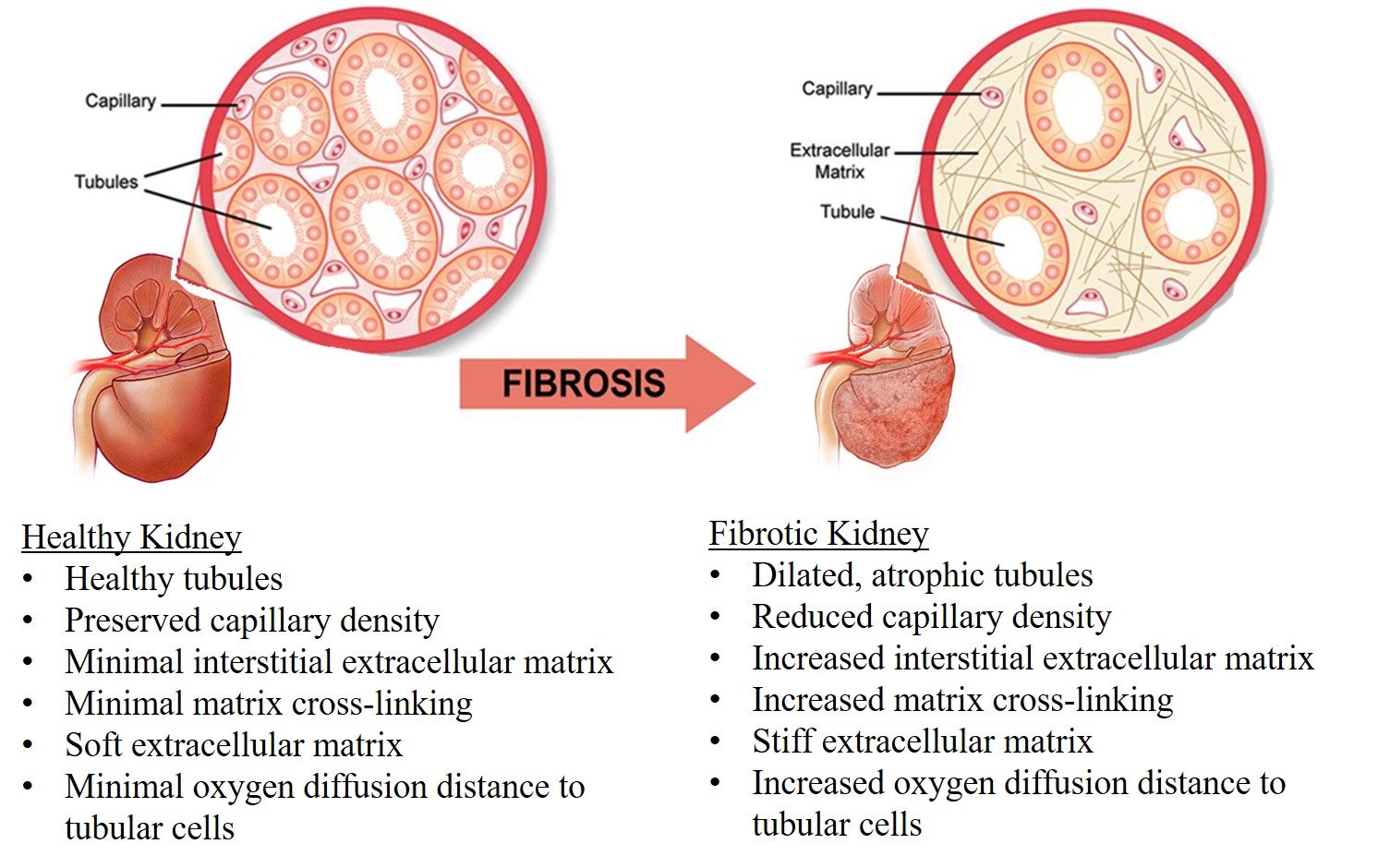
Kidney fibrosis, also known as renal fibrosis, is a condition where the kidneys develop scar tissue, leading to loss of kidney function, progression to end-stage kidney disease, increased risk of cardiovascular disease, and kidney failure. Kidney fibrosis is a common complication of chronic kidney disease (CKD), and the prevalence of CKD, which includes fibrosis, is significant globally. Approximately 10-14% of the global population is affected by CKD stages 1-5, and it is estimated that in the United States about 14% of adults have CKD. Several factors that may increase the risk of developing CKD include diabetes, high blood pressure, heart disease, obesity, family history, and older age. Additionally, certain ethnicities (Black, Native American, Asian American), smoking, and long-term use of certain medications, like NSAIDs, can also raise CKD risk.
Chronic Inflammation
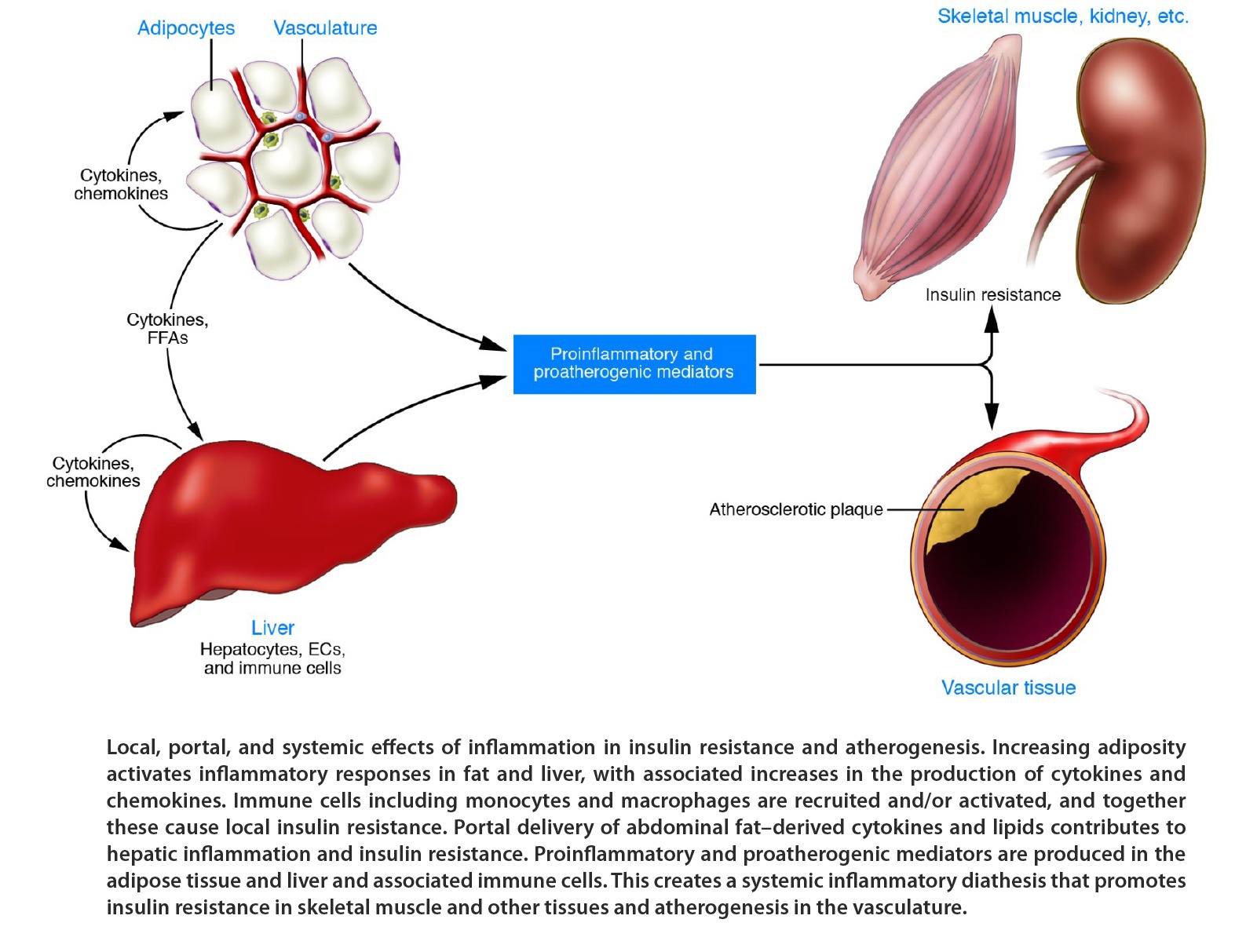
Chronic inflammation in many tissues and organs often results in irreversible damage and poor quality of life due to pain, organ failure, and morbidity. Most prevalent anti-inflammatory drugs are steroids and non-steroidal anti-inflammatory drugs (NSAIDs). Unfortunately, the chronic long-term use of these drugs may result in severe side effects that makes their use limited. Recently developed biologics that are prescribed for controlling inflammation can result in dampening of the patient’s normal immune responses to foreign agents and cancer. We have identified anti-inflammatory oxysterol drug candidates that act through different mechanisms than those of steroids and NSAIDs, and as such hold promise for being safe when used long-term. Oxy210 is one such anti-inflammatory oxysterol that controls chronic inflammation by targeting macrophages in preclinical models of MASH, atherosclerosis, and obesity. Obesity is a risk factor for several chronic inflammatory conditions, including atherosclerosis, MASH and metabolic inflammation of fat tissue. Inflammation in fat tissue can result in insulin resistance which leads to diabetes.
Inflammaging is a term that describes the chronic, low-grade inflammation that is a characteristic feature of the aging process. It is a significant factor in the development of chronic age-related diseases, including cardiovascular disease, diabetes, cancer, neurologic disorders, and overall decline in health. Unlike acute inflammation, which is a natural response to injury or infection, inflammaging is a sustained, low-intensity state of inflammation. Several key factors contribute to inflammaging, including cellular senescence, mitochondrial dysfunction, and damage to cellular components. There is a great interest in mitigating the effects of inflammaging and improving overall health and longevity. Utilization of anti-inflammatory oxysterols, given their oral bioavailability, differentiated mechanism of action, anticipated safety and tolerability with long-term use, and inexpensive production may be an effective strategy for targeting inflammaging.
Figure derived from: Shoelson SE, Lee J, Goldfine AB. Inflammation and insulin resistance. J Clin Invest 116:1793-1801; 2006
Atherosclerosis
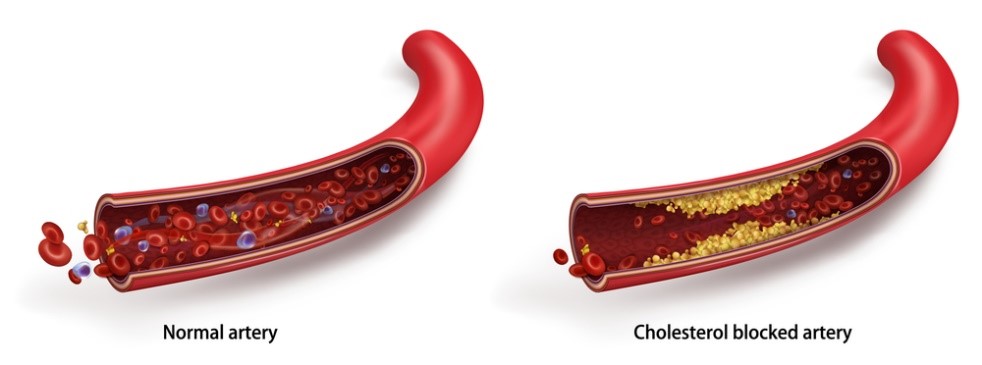
Cardiovascular disease (CVD) is common not only in the United States (US) but also worldwide. Atherosclerosis is known to be the major cause of CVD and its complications, including coronary artery disease (e.g., heart attack, heart failure, etc.), peripheral vascular disease and stroke. Atherosclerosis is characterized by gradual accumulation and modification of low-density lipoprotein cholesterol (LDL-C) in the artery walls, which eventually results in the formation of plaques that can rupture and obstruct blood flow, causing heart attack and stroke. Atherosclerosis is also known as a chronic inflammatory condition because of the involvement of pro-inflammatory immune cells, so-called macrophages, that are recruited to the blood vessel wall to remove the modified cholesterol products. However, in this process the macrophages often become loaded with toxic lipids and die before they can exit the vascular wall, resulting in the formation of atherosclerotic plaques.
According to the American Heart Association, approximately 121.5 million adults in the US may suffer from CVD, a leading cause of death for both men and women. About one in 58 people, or 4.6 million Americans, are directly affected by atherosclerosis in the US, although atherosclerosis is often symptom-free prior to the onset of CVD. Coronary artery disease alone accounts for approximately 610,000 deaths in the US annually, about 1 in 4 deaths. Nearly 735,000 Americans suffer heart attacks each year. Stroke is the number 5 cause of death globally and a leading cause of disability in the US: nearly 795,000 people suffer from stroke every year in the US, resulting in about 140,323 deaths.
Despite the positive impact cholesterol lowering drugs, such as statins, and lifestyle changes have had on treatment of atherosclerosis, the mortality from CVD is expected to increase from over 17 million in 2018 to almost 24 million by 2030 globally, and there continues to be a great unmet medical need for more effective and safe therapies. The market for anti-atherosclerosis drugs is expected to grow by over $3 billion USD between 2022-2026. Small molecule drugs, such as statins, that can reduce risk of atherosclerosis associated complications, are projected to see a significant amount of the growth over biologics.
At MAX BioPharma we have identified proprietary small molecule semi-synthetic oxysterols, exemplified by our lead molecule Oxy210. Oxy210 significantly inhibits atherosclerosis that develops in parallel with MASH in a hyperlipidemic humanized mouse model. This effect is likely due to anti-inflammatory and cholesterol lowering effects of Oxy210. Oxy 210 is orally bioavailable and has favorable pharmacokinetic and safety profiles. Oxy210 displays its anti-inflammatory effects in macrophages and vascular endothelial cells in part through inhibition of toll-like receptor signaling.
In recent years, in addition to classic risk factors for atherosclerosis, namely diabetes, hypercholesterolemia, hypertension and smoking, a significant correlation between non-alcoholic fatty liver disease (MAFLD), especially non-alcoholic steatohepatitis (MASH), and atherosclerosis has been reported. Patients with MAFLD and MASH die from CVD more frequently than from liver disease. In fact, MAFLD and MASH, are now considered independent, and likely causal, risk factors for the development of atherosclerosis. It has been therefore proposed that therapies that treat MAFLD may also inhibit atherosclerosis, especially since these diseases share common underlying factors including inflammation, lipid deposition and oxidation, and dysfunctional macrophages.
Oncology
Treatment of lung cancer remains an unmet medical challenge. Lung cancer is the leading cause of cancer death in the US. The American Cancer Society has estimated that in 2025 in the US, 226,650 people (110,680 men and 115,970 women) will be diagnosed with lung cancer, and that 124,730 people will die of lung cancer. On average, 1 in every 17 men and 1 in every 18 women will develop lung cancer. Because the symptoms of lung cancer often do not appear until the disease is already at an advanced stage, this may delay the diagnosis and give the disease a chance to progress. Despite many available generic treatment options, such as chemotherapy, radiation therapy, and surgery, and more specific therapies such as targeted therapy and immunotherapy, lung cancer continues to be associated with poor prognoses and a lower five-year survival rate than many other forms of cancer. For advanced metastatic lung cancer, the five-year survival rate remains low, at less than 3 percent. Metastasis and drug resistance are known to be major causes of failure in lung cancer therapy. New medicines are needed to not only inhibit tumor growth but also reduce invasive activity and metastasis and help overcome drug resistance in lung cancer patients.
Pancreatic cancer is the third leading cause of cancer death in the US and is expected to become the second leading cause by 2030. The American Cancer Society has estimated that in 2025 in the US, 67,440 people (34,950 men and 32,490 women) will be diagnosed with pancreatic cancer, and that 51,980 people will die of pancreatic cancer. As US population demographics change, the number of new cases of pancreatic cancer is expected to increase more than 2-fold and the number of deaths will increase 2.4-fold by the year 2030. Because the pancreas is located deep in the abdomen, early detection of this cancer is often difficult. In addition, pancreatic cancer tends to readily metastasize, even in early stages of the disease. Complete surgical removal of the tumor is possible in only about 18% of patients with the most common type of pancreatic cancer. Chemotherapy or chemotherapy with radiation and drug therapies are available, but five-year survival rates remain low, at less than 3 percent.
Bone Defects
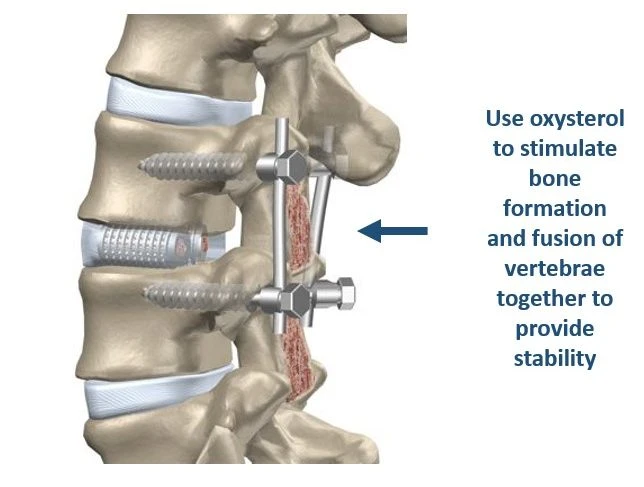
Spinal fusion is a prevalent procedure performed by orthopedic surgeons and neurosurgeons in order to address spinal deformities and provide stability. Over 400,000 spinal fusion surgeries are performed annually in the US. This number is expected to increase significantly over the coming years. Annually, the aggregate hospital cost associated with spinal fusion surgeries surpasses $13 billion, the highest of any surgical procedure. Of course, poor clinical outcomes, such as ‘failed fusions’, not only add to this high cost but also cause immense setbacks in patients who often must suffer through repeated surgeries. For example, failed fusions can occur in up to 40% of spinal fusion surgeries using autologous bone grafts, even when grafting the patient’s own iliac crest bone, the so called “gold-standard” for these procedures.
That is why the use of osteoinductive growth factors in bone graft materials, such as recombinant human bone morphogenetic protein 2 (rhBMP2), has become popular, particularly for spinal fusion procedures. However, rhBMP2 is produced using expensive recombinant DNA technology and carry their own set of risks, such as uncontrolled or ectopic bone formation, among others. We have identified Oxy133, a semi-synthetic osteogenic compound with excellent osteoinductive properties that stimulates bone formation through a different and effective bone forming mechanism than rhBMP2. Oxy133 is an oxysterol-based small molecule, inexpensive and readily produced (compared to recombinant human proteins), shelf stable and easy to use during orthopedic procedures. Oxy133 stimulates bone formation by selectively targeting mesenchymal stem cells as well as other osteoprogenitor cells in the body through allosteric activation of the osteoinductive Hedgehog signaling pathway. Under the right conditions, these cells can transform themselves and help form and repair certain tissues, such as bone, muscle, fat and cartilage. Oxy133 can induce mesenchymal stem cells to differentiate exclusively into bone forming cells (osteoblasts), and prevents them from converting into fat cells (unlike rhBMP2 that stimulates the formation of both bone and fat cells). In humans, the formation of new fat cells in bone often occurs at the expense of bone forming osteoblasts, especially as we age. We believe that Oxy133 could enter the market as a viable alternative to rhBMP2 (Infuse®), a leading product on the market for spinal fusion despite its less than favorable safety profile and high cost, and other bone graft materials and lead to improved patient safety and outcomes. We have demonstrated robust bone formation by Oxy133 in animal models of spinal fusion, such as in rat and rabbit models as well as the healing of cranial, maxillofacial, and long-bone defects. The target of Oxy133 was identified as the allosteric site of the smoothened receptor that stimulates bone formation through activation of Hedgehog signaling in mesenchymal stem cells. Under the guidance of BCVG, we’ve completed a pre-sub and a Q-sub meeting with the Food and Drug (FDA), during which the agency determined that Oxy133 will be designated a device.
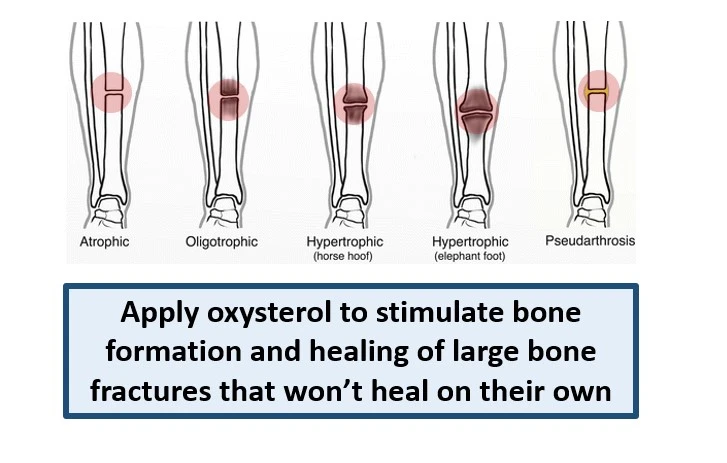
Another application of Oxy133 is in the area of non- or poorly-healing bone fractures. In some patients, broken bones do not readily knit back together naturally for several reasons. For example, the fracture may be too severe, the patient may be diabetic, suffer from osteoporosis, or may be a heavy smoker, among other factors. A surgeon repairing such fractures may have to graft bone from elsewhere in the body or use cadaver bone to stimulate bone formation and fracture healing. In this context, Oxy133 could be used to induce bone formation around the fracture to knit the bones back together naturally.
 Oxy133 could potentially be used to help trauma patients recovering from injuries to their facial or head bones. The natural and unaided healing of such injuries can be incomplete or defective, resulting in gaps where fractured bones did not heal or regenerate completely. Oxy133, used alone or in combination with mesenchymal stem cells, incorporated in a scaffold could be placed in a bone defect to regenerate bone. We have demonstrated robust bone formation by Oxy133 in animal models of cranial and maxillofacial bone defects.
Oxy133 could potentially be used to help trauma patients recovering from injuries to their facial or head bones. The natural and unaided healing of such injuries can be incomplete or defective, resulting in gaps where fractured bones did not heal or regenerate completely. Oxy133, used alone or in combination with mesenchymal stem cells, incorporated in a scaffold could be placed in a bone defect to regenerate bone. We have demonstrated robust bone formation by Oxy133 in animal models of cranial and maxillofacial bone defects.
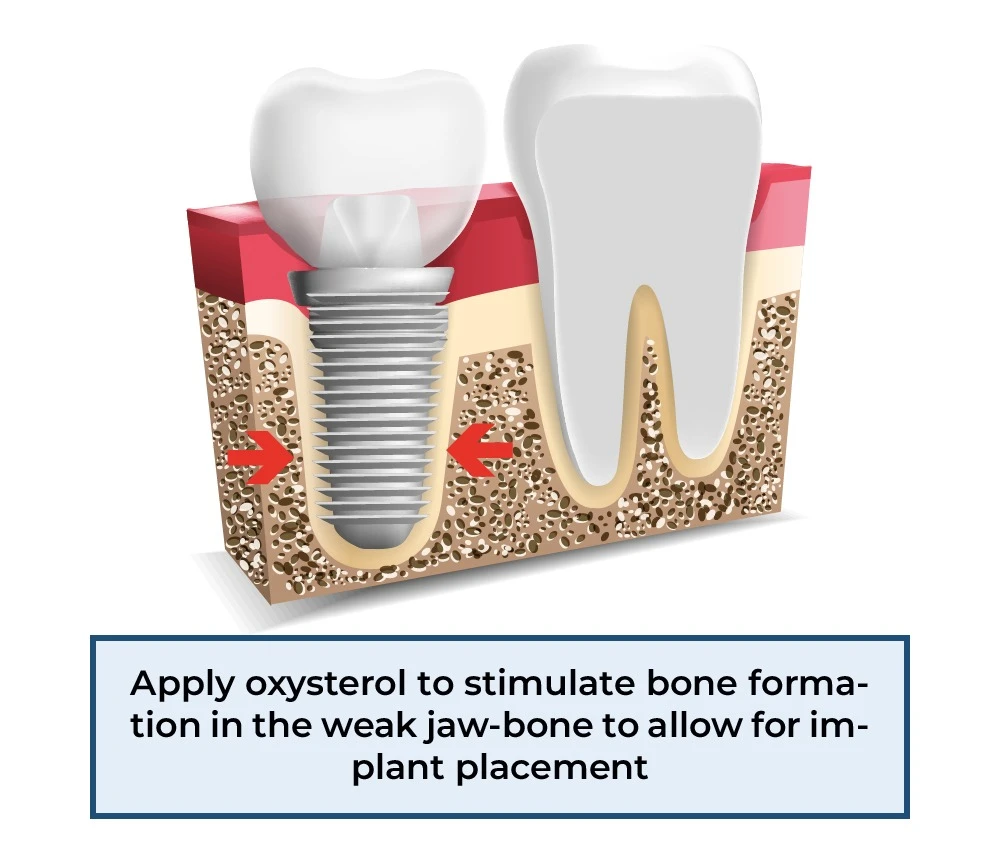 For dental patients in need of implants, the use of osteogenic oxysterols such as Oxy133 could have a significant positive impact. Often, dental patients have lost too much bone in their jaw to allow for an implant to be secured. Instead of using cadaver bone or bone harvested from the patient, a formulation of MAX BioPharma’s proprietary osteoinductive oxysterols may stimulate bone formation and strengthen the areas where implants can be placed.
For dental patients in need of implants, the use of osteogenic oxysterols such as Oxy133 could have a significant positive impact. Often, dental patients have lost too much bone in their jaw to allow for an implant to be secured. Instead of using cadaver bone or bone harvested from the patient, a formulation of MAX BioPharma’s proprietary osteoinductive oxysterols may stimulate bone formation and strengthen the areas where implants can be placed.
Microbial Infections
The Covid-19 pandemic has impacted human health and wellbeing worldwide. Safe and effective drug treatment options for Covid-19 are still needed to help vulnerable patients. Remdesivir (Veklury) and nirmatrelvir/ritonavir (Paxlovid) are FDA approved drugs to treat Covid‑19; however, these drugs are not without side effects. Through a research collaboration with the National Institute of Infectious Diseases in Tokyo, Japan, we and our colleagues have demonstrated that some oxysterols can prevent different strains of the SARS-CoV-2 virus from replicating in cell culture and human lung organoids.
Patients with chronic HBV infections are at increased risk of developing significant liver disease, including cirrhosis (permanent scarring of the liver), as well as liver failure and liver cancer. The Hepatitis B Foundation estimates that more than 884,000 people die every year due to the consequences of hepatitis B disease. Although HBV infection is the most common liver infection in the world; most patients fully recover and avoid chronic HBV infection. However, nearly 300 million people worldwide are chronically infected with HBV, including more than 2 million Americans, according to figures published by the Hepatitis B Foundation.
Tuberculosis (TB), caused by infection with Mycobacterium tuberculosis (Mtb), remains a global health threat with a high death toll every year. An estimated 1.3 million people died from TB in 2023, and better control and management of TB is one of the most urgent and difficult challenges facing global health. The current standard of care for non-drug resistant or drug sensitive TB treatment can take at least 4-9 months, causing significant adverse effects and increasing the risk of non-adherence. Mtb can survive in the human body for a prolonged period and is responsible for chronic and recurrent infections, especially among immunocompromised TB patients. The necessity for novel antibiotics with a unique mechanism of action that contributes to the diversification of the current antibiotic arsenal, and can disrupt bacterial resistance, would provide a strategic therapeutic advantage.
In collaboration with scientists at Metaba, LLC, we have identified orally bioavailable, novel semi-synthetic oxysterols with Mtb bactericidal activity. As a new chemical class of antibiotics, oxysterol-based therapies may be less vulnerable to resistance since factors that cause resistance, including mutations and enzymes that destroy conventional antibiotics, are unlikely to target them. Oxysterols may become a novel chemical family of next generation antibiotics to combat not only Mtb but also other pathogenic bacteria.